Chronic Obstructive Pulmonary Disease
Definition of COPD
Emphysema
– loss of elastic recoilAsthma
– reversible anatomic airway narrowingBronchiectasis/Cystic Fibrosis
– irreversible anatomic airway narrowingChronic Bronchitis
– anatomic airway narrowingFunctional Abnormalities of COPD
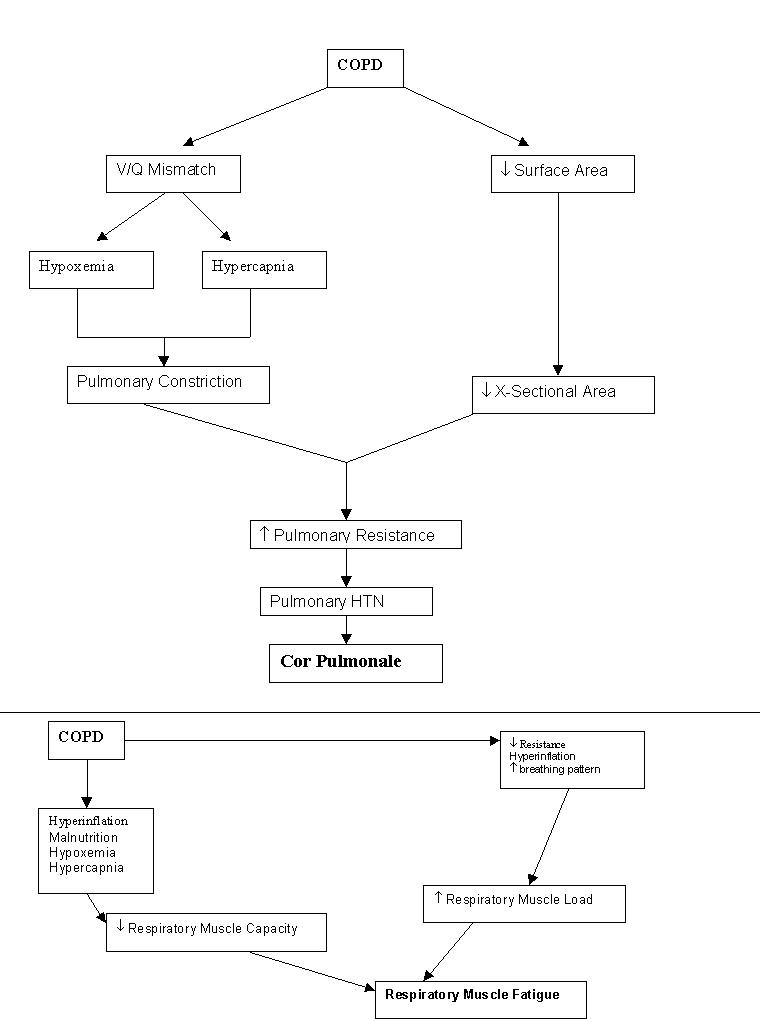
Mechanism of Cor Pulmonale and Respiratory Muscle Fatigue in COPD

Physical Findings of COPD
Treatment of COPD