Abdominal Cavity
peritoneal cavity: subset of the abdominal cavity lined by continuous serous membrane called peritoneum
- peritoneal cavity is really only a potential space; may be filled in pathologic conditions (i.e. ascites)
- peritoneum is separated from the transversalis fascia by a fatty layer (extraperitoneal fat)
- visceral and parietal peritoneum and mesentaries are all one continuous membrane
- arietal peritoneum: lines the abdominal wall
- visceral peritoneum: forms outer, serous covering of organs
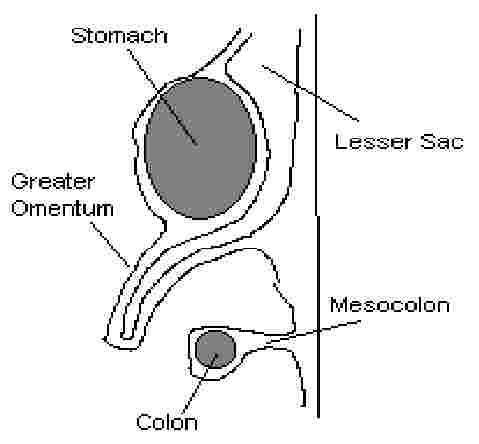
greater and lesser sacs (bursa): the peritoneum is divided into two developmental spaces
- greater sac is larger and contains the peritoneal organs (remnant of left pleuroperitoneal space)
- lesser sac is retrogastric and is a potential space (remnant of right pleuroperitoneal space)
Omental Foramen (Epiploic Foramen of Winslow): connects the sacs Þ potential herniation site
- anterior boundary
: free edge of lesser omentum (portal vein, hepatic artery, bile duct)
- posterior boundary
: IVC, crus of diaphragm
- superior boundary
: liver
- inferior boundary
: duodenum, portal vein, hepatic artery, bile duct
mesentaries: double layer of peritoneum formed by punching in of organs during development (see fig)
- named for organs it covers (i.e. mesocolon, mesogastrium)
- connects organs to abdominal wall, but allows them to be mobile
- blood vessels, nerves and connective tissue are sandwiched between the two layers of the mesentary
peritoneal ligaments: structures analogous to mesentaries connecting two organs (i.e. gastrosplenic ligament connnects stomach to spleen)
intraperitoneal structures: enveloped by the peritoneum and attached to abdominal wall by mesentaries
- stomach, 1st part of duodenum, jejunum, ileum, cecum, appendix, transverse colon, sigmoid colon, liver (except bare area), spleen
primarily retroperitoneal: never surrounded by peritoneum
- kidneys, aorta, IVC, rectal canal, ureters, suprarenal glands
secondarily retroperitoneal: initially were intraperitoneal, but through development became apposed and fused to the abdominal wall either directly or through apposition of the mesentary
- ascending and descending colon, duodenum (parts 2-4), head and body of pancreas
peritoneal recesses: blind pouches (potential spaces) formed by the complex folding of the peritoneum
- potential sites of fluid (or pus, feces, etc) accumulation; provide surgical access; potential hernia sites
greater omentum: fatty, 4-layered ‘apron’ formed by a large flap of mesentary folded onto itself and fused together (see fig)
- connects stomach to posterior abdominal wall and diaphragm
- hangs down off greater curvature of stomach and covers intestines
- secretes and absorbs peritoneal fluid; source of macrophages
- has mobility, can seal off inflamed areas of the peritoneum to prevent spread of infections; remnant of dorsal mesentery
lesser omentum: connects lesser curvature of stomach and duodenum to the liver
- contains hepatogastric ligament, hepatoduodenal ligament
- remnants of ventral mesentary
four parts of duodenum – 1st is movable, others are immobile
accessory and main pancreatic duct (pancreatic and bile duct) – into 2nd part of duodenum
suspensory ligament (ligament of Treitz) – smooth and striated muscle at junction of duodenum and jejunum
Structures
peritoneum: lines the abdominal cavity
peritoneal cavity: formed by peritoneum (closed sac except in infundibulum of each uterine tube in females)
serous coat: outer lining of peritoneum that covers an organ when it invaginates the peritoneum
peritoneal folds (plicae): peritoneum with a free edge raised up off of the abdominal wall, usually by a vessel or
- ligament running between the peritoneum and the abdominal wall
medial umbilical folds: cover medial umbilical ligaments (obliterated umbilical arteries)
median umbilical fold: covers median umbilical ligament (remnant of urachus)
lateral umbilical folds: cover inferior epigastic arteries
lesser omentum: connects lesser curvature and duodenum to the liver – has two parts:
hepatogastric ligament: connects liver and stomach
hepatodudenal ligament: connects liver and duodenum
greater omentum: hangs from greater curvature; mesentary doubled back to give a four-layer flap of peritoneum
mesentary: double layer of peritoneum formed by punching in of organ from posterior abdominal wall
- attaches organ to abdominal wall; allows movement; blood vessels and nerves run between folds
ligamentum teres: free edge of falciform ligament (remnant of umbilical vein)
diaphragm: note the extent of the doming Þ wounds can potentially penetrate both the peritoneum and pleura
liver:
- falciform ligament
: divides liver into two lobes (right and left); attaches liver to anterior abdominal wall
- bare area of liver
: pertioneum reflects away from the liver in the posterior leaving an uncovered area
- coronary ligament
: peritoneal reflections around bare area; ligament running along superior margin of liver
- right and left triangular ligament
: right and left portion of coronary ligament, respectively
gall bladder: protrudes beyond the inferior border of the liver; projects to the lateral margin of the rectus abdominus also contacts duodenum and large bowel
stomach:
- pylorus
: connects the stomach to the duodenum; identified as firm area by palpation
- greater and lesser curvatures
spleen: posterior to stomach, in contact with diaphragm
- gastrolineal (gastrosplenic) ligament: double layer of peritoneum; connects spleen and stomach
- head, neck, body, tail
small intestine: total length is 6 m
- duodenum: begins at pylorus; first part is intraperitoneal; second, third and fourth parts are retroperitoneal
- ligament of Treitz
: suspends fourth part of the duodenum at the duodenal-jejunal junction – connects to diaphragm at right crus
- jejunum
: proximal 2/5 of the mobile part of the small intestine
- ilium
: distal 3/5 of the mobile part of the small intestine; opens into superior part of cecum
large intestine:
- cecum: blind pouch at proximal end of large bowel; ileocecal junction is at superior part
- veriform appendix
: narrow, blind tube that connects to the cecum inferior to the ileocecal junction
- ascending colon
: retroperitoneal; has no mesentary
- transverse colon
: intraperitoneal; extends from right colic flexure to left colic flexure
- decending colon
: smaller diameter than ascending colon; retroperitoneal
- sigmoid colon
: has long mesentary and is very mobile
- rectum
: stores feces; only partially covered by peritoneum; actually considered part of pelvic region
- teniae coli
: muscles that run longitudinally along the colon; derived from longitudinal smooth muscle (three)
- haustra
: sacculations along the colon resulting because the teniae coli are shorter than the colon
- epiploic appendices
: small bags of visceral peritoneum filled with fat; hang off the colon along its length
- right colic flexure
: junction of ascending and transverse colon - at inferior tip of left lobe of the liver
- left colic flexure
: junction of transverse and descending colon - at inferior border of spleen
epiploic foramen of Winslow: connects greater and lesser peritoneal sacs (potential herniation site)
- anterior boundary: free edge of lesser omentum (portal vein, hepatic artery, bile duct)
- posterior boundary
: IVC, crus of diaphragm
- superior boundary
: liver
- inferior boundary
: duodenum, portal vein, hepatic artery, bile duct
root of mesentery: refers to mesentery of small intestine; runs obliquely from left side of L2 to the right sacroiliac joint
peritoneal gutters: mesentaries can form gutters that can conduct fluid around the peritoneal cavity
- right paracolic gutter: to the right of the ascending colon
- left paracolic gutter
: to the left of the descending colon
- right infracolic gutter
: to the left of the ascending colon
- left infracolic gutter
: to the right of the descending colon
hepatorenal recess: posterior to the liver, anterior to right kidney; site of fluid accumulation in supine position
subphrenic recess (right and left): anterior to liver, posterior to anterior abdominal wall

